
GERM Studies
Creators: E. Carlson, C. Fan, M. Forte, Y. Gao, L. Hershkowitz, E. Jeong, J. Kim, E. Pun, E. Yoon
Supervisor: Peter Yeadon
Collaborators: NYU Langone Medical Center & NBBJ New York & Yeadon Space Agency
Evidence teaches us that environmental contamination clearly plays an important role in the acquisition of nosocomial pathogens, so contemporary architects and designers must engage an assortment of considerations in creating healthcare products and environments: What materials are these spaces made of? How easy are they to isolate and disinfect? What equipment is necessary? How do pathogens spread, and how might they be tracked? What surfaces does one come into contact with? What protocols are required to clean specific materials? What is the length of turnover time between occupants in patient rooms? What surfaces are inherently resistant to contaminants? How can natural ventilation and/or mechanical ventilation help reduce infections
Concurrently, the evolution of antimicrobial environments in schools, hospitals, abattoirs, etc., has been propelled by the development of advanced nanomaterials for manufactured products that design professionals use. But these antimicrobial materials should not be thought of as a silver bullet that replaces good hand hygiene and proper protocols for cleaning/disinfecting interior environments.
In fact, a range of approaches will be needed in order to enhance our ability to combat hospital-associated infections (HAIs). We will need interior environments and medical devices that resist contamination, and we will also need to understand where antibiotic-resistant pathogens linger and how they spread.
Concurrently, the evolution of antimicrobial environments in schools, hospitals, abattoirs, etc., has been propelled by the development of advanced nanomaterials for manufactured products that design professionals use. But these antimicrobial materials should not be thought of as a silver bullet that replaces good hand hygiene and proper protocols for cleaning/disinfecting interior environments.
In fact, a range of approaches will be needed in order to enhance our ability to combat hospital-associated infections (HAIs). We will need interior environments and medical devices that resist contamination, and we will also need to understand where antibiotic-resistant pathogens linger and how they spread.
Research has demonstrated that a person admitted to a hospital room previously occupied by a patient with methicillin-resistant Staphylococcus aureus (MRSA) or vancomycin-resistant enterococci (VRE) significantly increases the odds of acquiring MRSA and VRE. The sources of transmission are: patients, healthcare workers, and environmental contamination. Even after cleaning, floors, beds, gowns, tables, faucets, doorknobs, pressure cuffs and digital devices remain stubbornly contaminated.
Reports also show that, on average, healthcare workers frequently come into contact with dozens of surfaces every time they interact with a patient. Bed rails, bed surfaces, over-bed tables, intravenous pumps, and supply carts are considered to be the highest touched surfaces during these interactions.
Because pathogens can persist in the environment for several days to several months, and because there is evidence that only half of approximately 20,000 surfaces (14 types of objects) might be disinfected during a terminal room cleaning, environmental sensors will increasingly become a vital tool in communicating and understanding where threats lie.
To address these threats as a group of students, faculty, and professionals, our GERM Studies team began with careful observations in the field, in order to gain an understanding of some of the significant challenges that HAIs present.
Reports also show that, on average, healthcare workers frequently come into contact with dozens of surfaces every time they interact with a patient. Bed rails, bed surfaces, over-bed tables, intravenous pumps, and supply carts are considered to be the highest touched surfaces during these interactions.
Because pathogens can persist in the environment for several days to several months, and because there is evidence that only half of approximately 20,000 surfaces (14 types of objects) might be disinfected during a terminal room cleaning, environmental sensors will increasingly become a vital tool in communicating and understanding where threats lie.
To address these threats as a group of students, faculty, and professionals, our GERM Studies team began with careful observations in the field, in order to gain an understanding of some of the significant challenges that HAIs present.

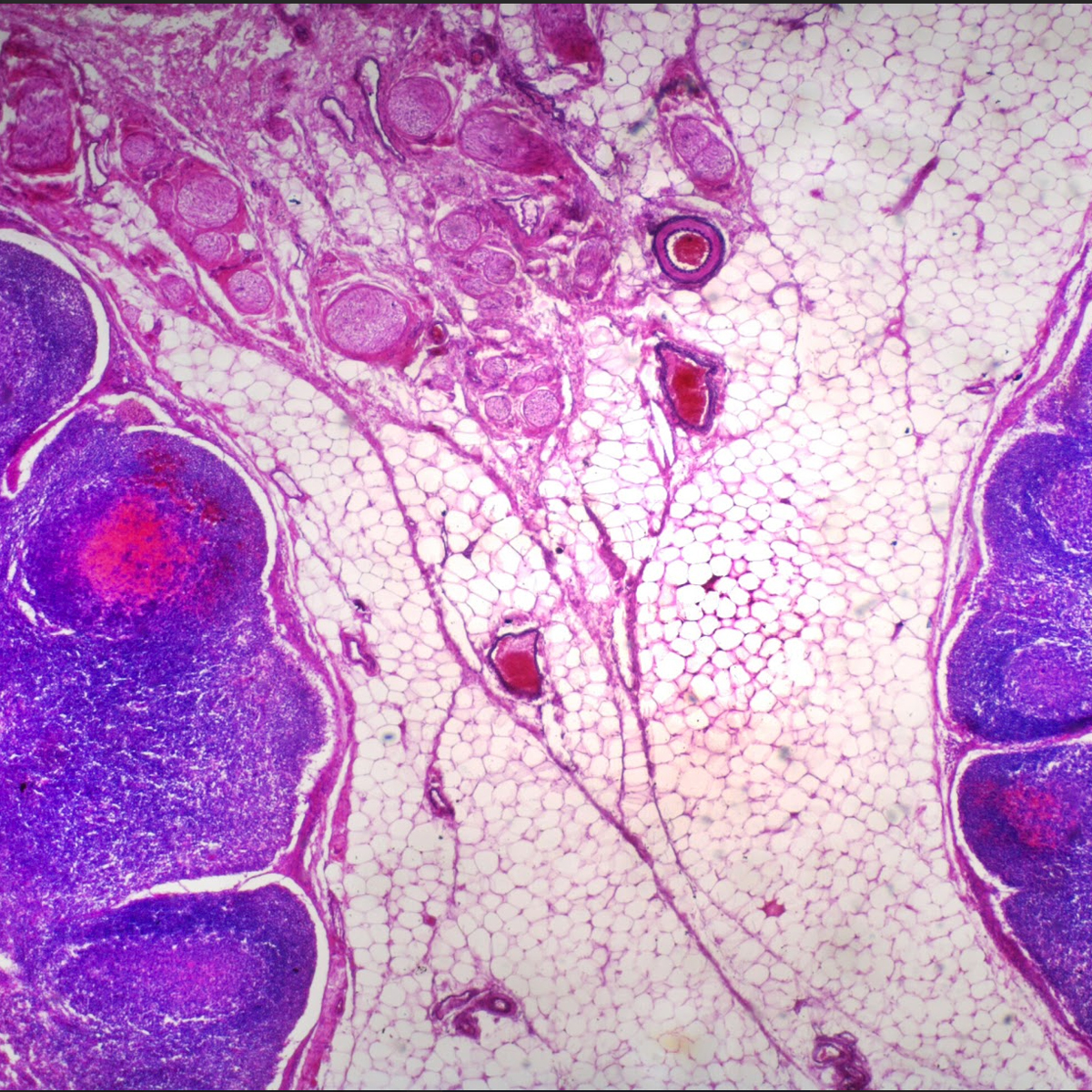
In the design and construction of environments that support infection prevention, there are a variety of elements and factors that are worthy of study. As others have stressed, the key is to connect critical thinking skills with published evidence and experience gained in the field.
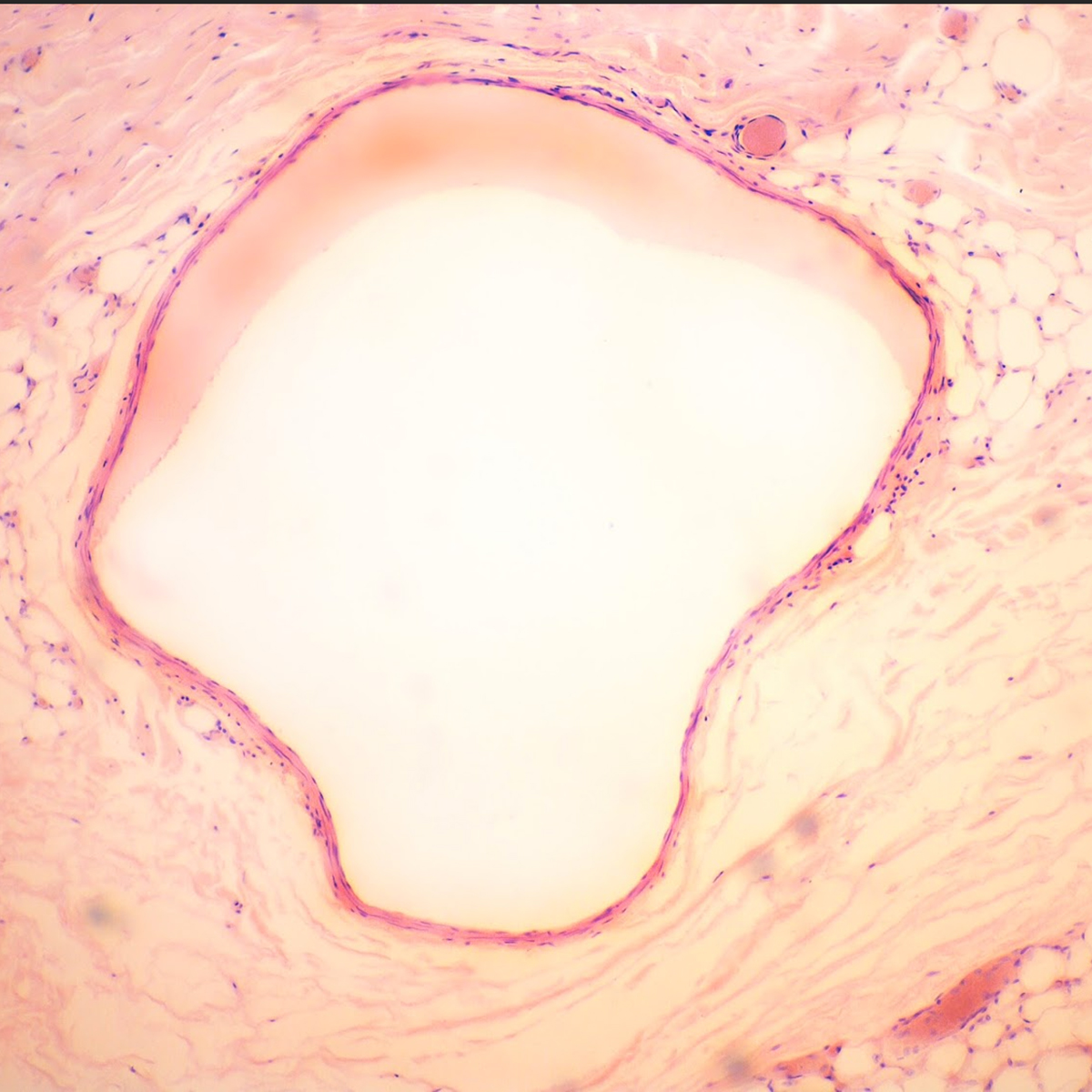
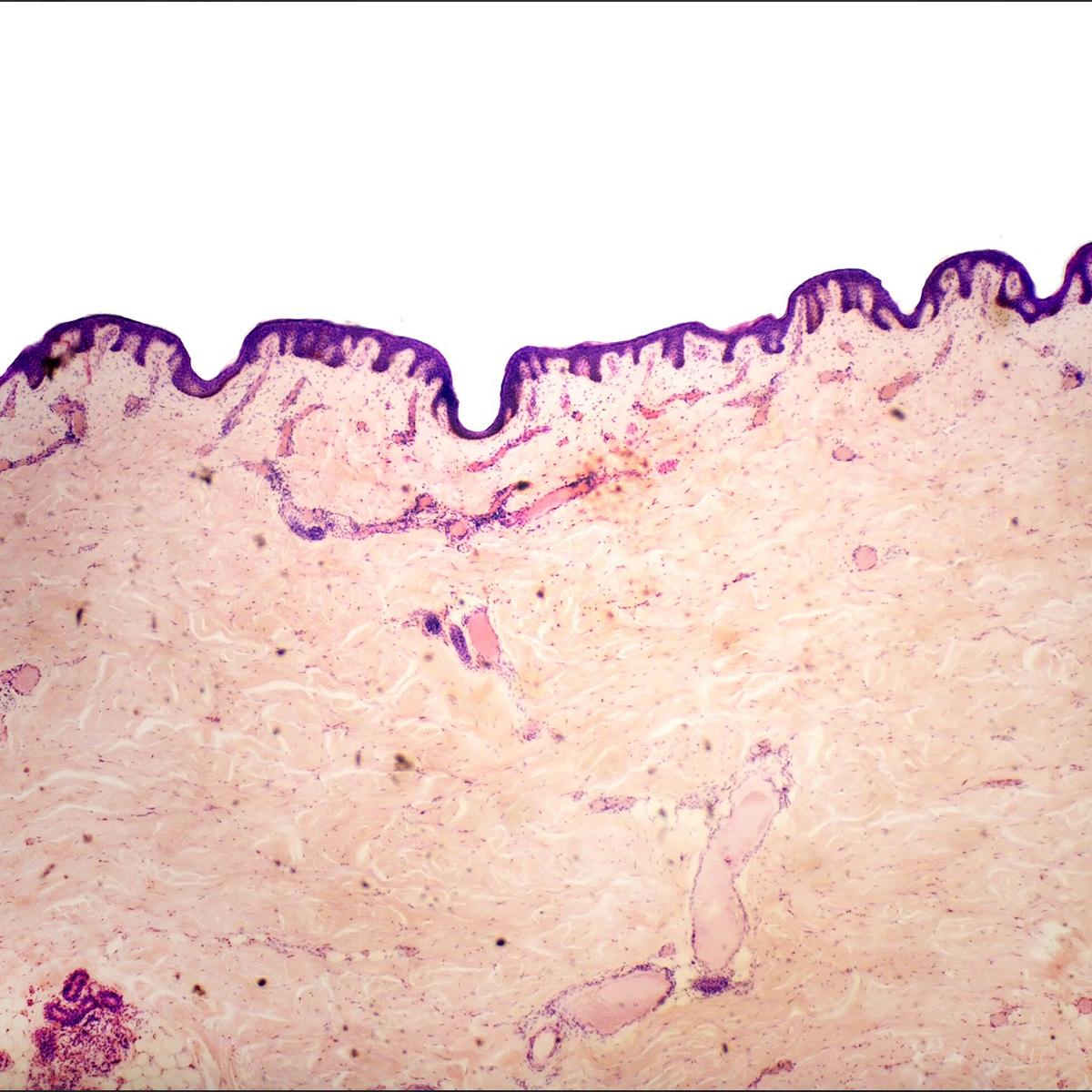
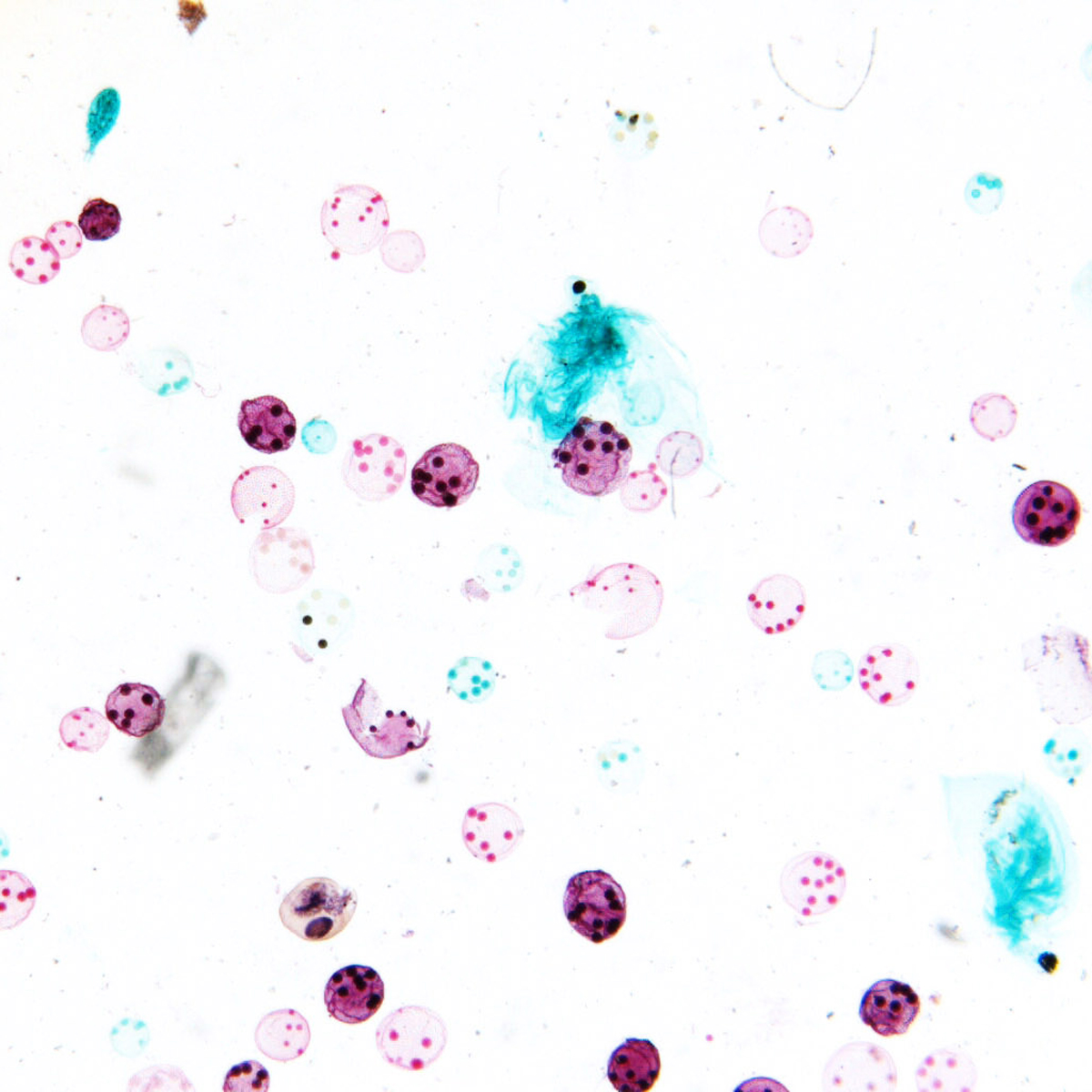
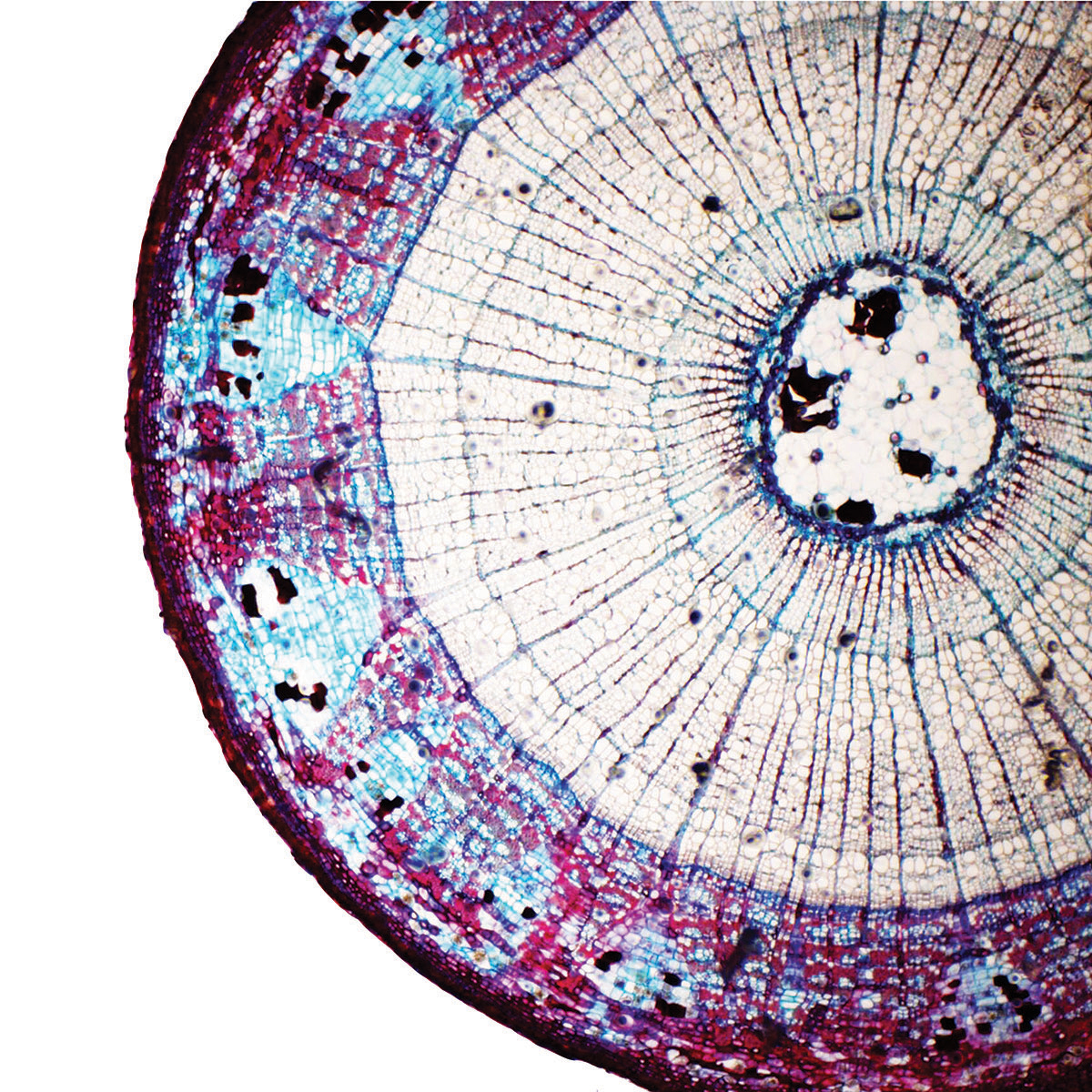
This approach was fundamental to our GERM Studies. Working with experts from NYU Langone Medical Center and NBBJ New York, our team collected samples of microorganisms from the field, then incubated, fixed, stained, and imaged the bateria samples. A selection of those images is presented above.
This approach was fundamental to our GERM Studies. Working with experts from NYU Langone Medical Center and NBBJ New York, our team collected samples of microorganisms from the field, then incubated, fixed, stained, and imaged the bateria samples. A selection of those images is presented above.
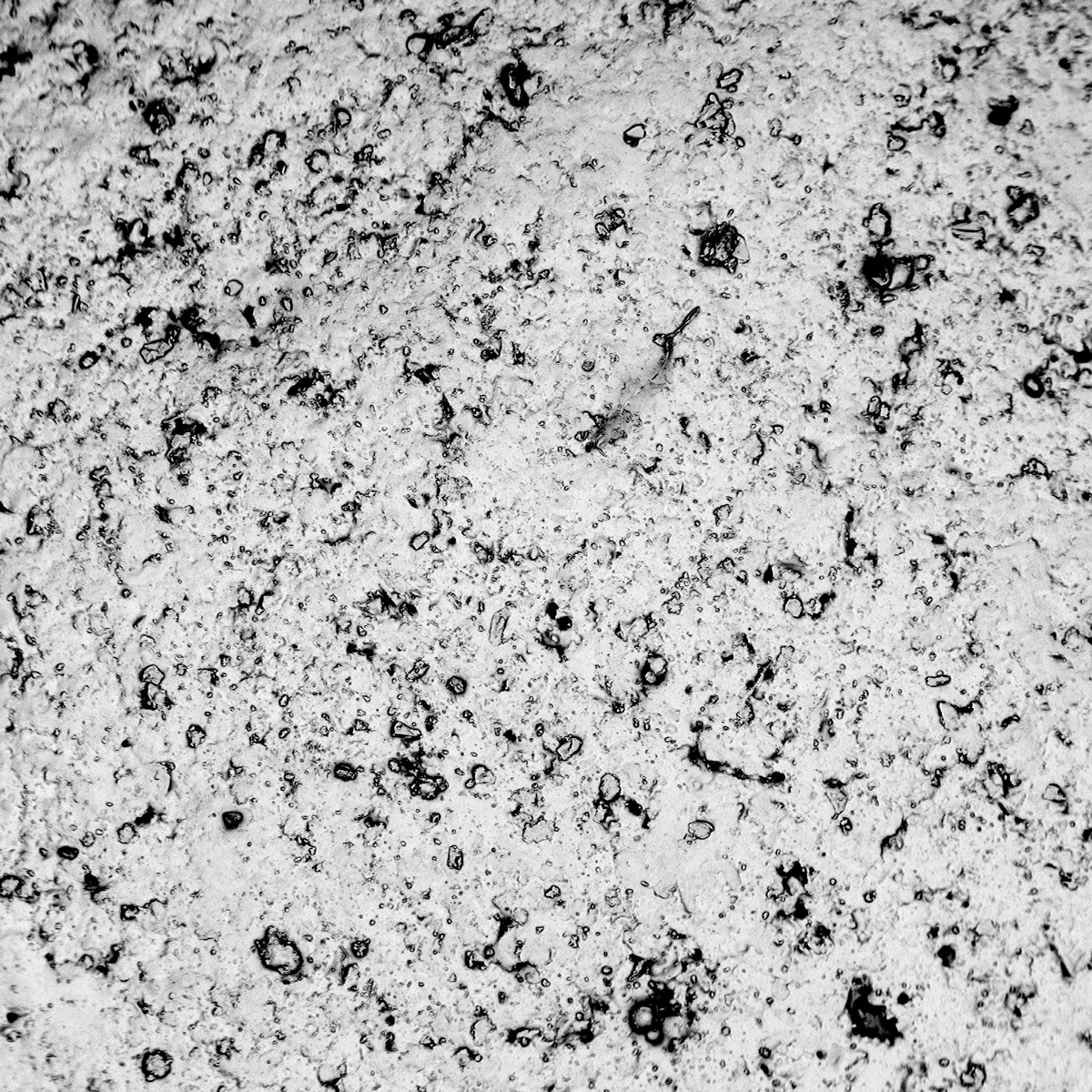
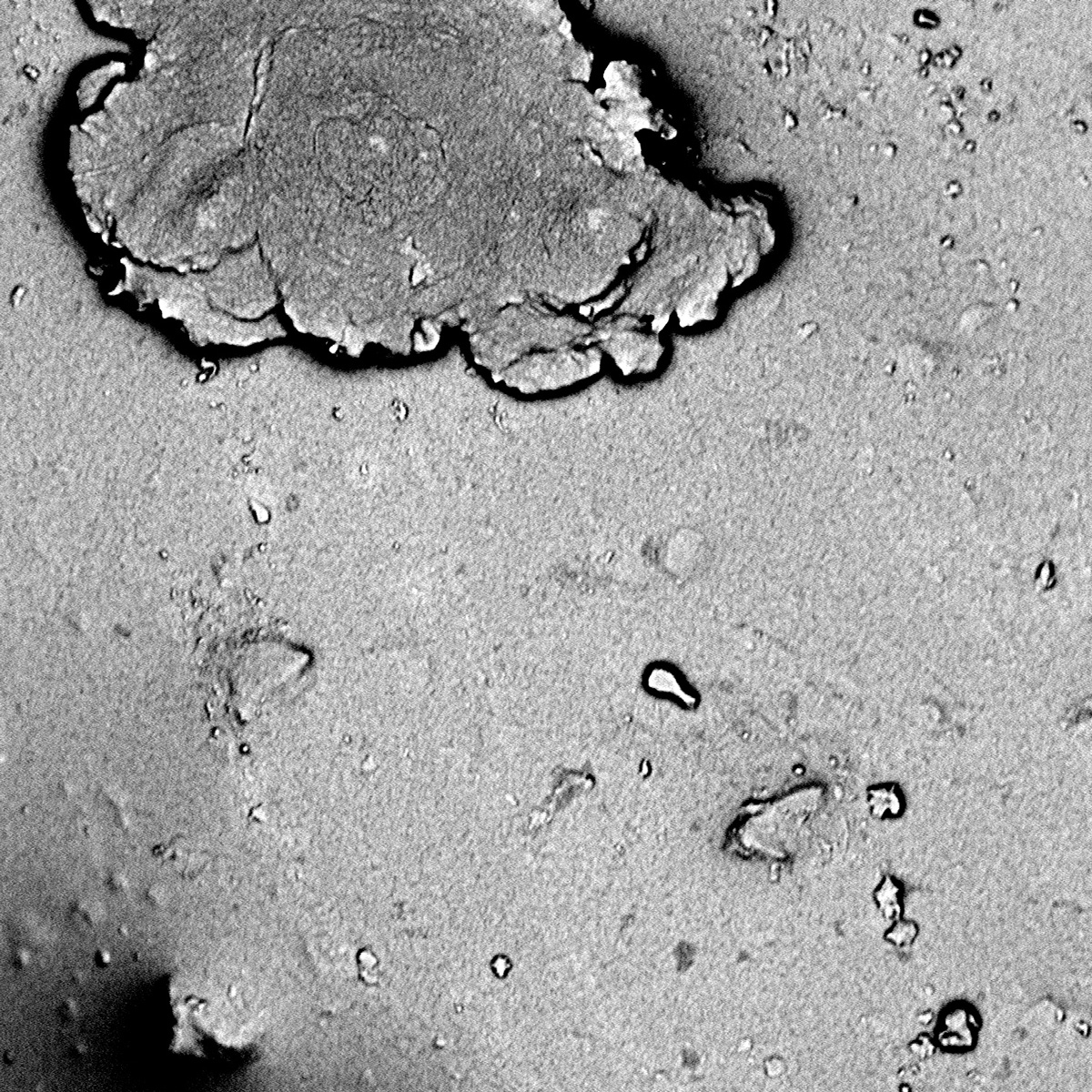
We also used RISD’s electron microscope to study the surface topographies of many common materials that are used in products and the built environment, which microorganisms can attach to, such as: bandages (Walgreens), face masks (Safety Products), PTFE (Sun Sri), bedding (IKEA), HDPE, bioplastic composites (Yeadon Space Agency), ceramic tiles (Walker Zanger), acrylic panels (3Form), and glass (Walker Zanger). And, we imaged a selection of antimicrobial materials, such as: copper (3M), polyurethane foam with Microban, acetal copolymers with Anti-Crobe, synthetic mats with Microban, and Sharklet. Some of those images are presented below.






Previous Next
Back︎︎︎

